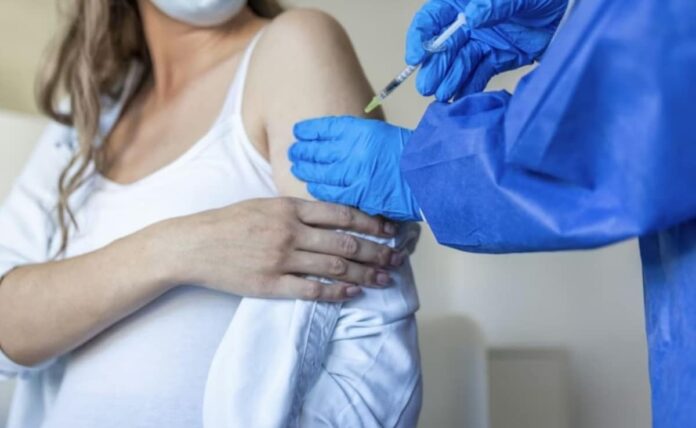
In what is being described as a visionary leap for women’s health in India, the government has officially commenced the nationwide rollout of the Human Papillomavirus (HPV) vaccine. Speaking on Thursday, V.M. Katoch, the former Director General of the Indian Council of Medical Research (ICMR), characterized the initiative as a “transformative” milestone that will finally protect the most vulnerable segments of the population.
Cervical cancer claims the lives of thousands of Indian women annually, often during their most productive middle years. By making the vaccine a part of the national mandate, India aims to follow the global blueprint for cancer elimination.
Also Read | Imran Khan and Bushra Bibi Sentenced to 17 Years in Jail
Bridging the Two-Decade Gap: From Private to Public
While the HPV vaccine was approved for use in India nearly 20 years ago, it remained largely out of reach for the general public.
-
The Wealth Barrier: High costs meant that only those utilizing private healthcare could afford the multi-dose regimen.
-
Economic Inequity: Consequently, girls from lower-income families remained disproportionately at risk.
-
National Inclusion: The new rollout ensures that the vaccine is provided free of cost or at highly subsidized rates through government health centers, mirroring the success of over 160 other nations.
The Science of Prevention: Targeting the Root Cause
Cervical cancer is unique because its primary cause—HPV infection—is preventable through timely immunization.
-
High Efficacy: The vaccine has a proven global track record of significantly reducing the incidence of pre-cancerous lesions.
-
Community Immunity: Widespread vaccination not only protects the individual but also reduces the overall transmission of the virus within the community.
Also Read | Imran Khan and Bushra Bibi Sentenced to 17 Years in Jail
The Roadmap to Elimination
Katoch expressed confidence that this move is the first step toward a cervical cancer-free India. By targeting young girls before they are exposed to the virus, the program seeks to create a “milestone of prevention” that will be felt for generations.
Reality Check
The nationwide rollout is an incredible feat of logistics. Still, the success of the program depends entirely on public awareness and overcoming vaccine hesitancy. In fact, despite the vaccine’s safety record, myths regarding its impact on fertility often circulate in rural areas. Therefore, while the supply of the vaccine is now a landmark achievement, the uptake will require a massive communication drive from the Ministry of Health.
The Loopholes
The vaccine is now part of the national program. In fact, this is a “Timing Loophole”—while the vaccine is highly effective for young girls (typically ages 9–14), it offers much lower protection for older women who may have already been exposed to HPV. Therefore, the “landmark step” primarily protects the next generation, while the current generation of adult women still requires regular screening (Pap smears/HPV DNA tests). Still, the “Implementation Loophole” remains; ensuring consistent cold-chain storage for these vaccines in remote rural areas will be the program’s biggest hardware challenge.
Also Read | Imran Khan and Bushra Bibi Sentenced to 17 Years in Jail
What This Means for You
If you have a daughter between the ages of 9 and 14, prioritize her vaccination now. First, realize that the vaccine is most effective before any exposure to the virus occurs. Then, if you are an adult woman, understand that while the vaccine may not be part of your age bracket’s free rollout, you should still discuss screening with your doctor every 3–5 years.
Finally, understand that the vaccine is safe. You should rely on official ICMR and WHO data rather than social media rumors. Before the next school year begins, check if your local government school or primary health center (PHC) has started the school-based vaccination drive, which is often the easiest way to ensure completion of the doses.
What’s Next
Expect a massive “Jan Andolan” (People’s Movement) campaign to be launched by the Ministry of Health by mid-2026. Then, look for the rollout of Ceravac (India’s first indigenous HPV vaccine) to further lower the procurement costs for the government. Finally, the WHO is expected to release a fresh report in 2027 to see if India’s inclusion has significantly tilted the global numbers toward the goal of eliminating cervical cancer by 2030.
Also Read | Imran Khan and Bushra Bibi Sentenced to 17 Years in Jail
End…